Children’s bodies are constantly growing and developing, which makes their health needs very different from those of adults. Blood plays a vital role in growth, immunity, oxygen transport, and healing. When something affects the blood system, it can impact a child’s energy levels, immune protection, and overall development.
The field of paediatric haematology focuses on diagnosing and treating blood diseases in children, including anaemia, leukaemia, clotting disorders, and genetic conditions such as thalassaemia. Early diagnosis and specialised treatment can significantly improve outcomes and quality of life for young patients.
In this guide, we explain common childhood blood disorders, the childhood leukaemia signs parents should know, and how specialists in paediatric haematology Pakistan are improving care through early screening and advanced treatment options.
What Is Paediatric Haematology?
Paediatric haematology is a specialized medical field dedicated to diagnosing and treating blood disorders in infants, children, and adolescents.
Blood contains several important components:
- Red blood cells – carry oxygen to tissues
- White blood cells – fight infections
- Platelets – help blood clot and prevent bleeding
- Plasma – carries nutrients and proteins
When one or more of these components become abnormal, a child may develop a blood disorder.
Research shows that childhood blood disorders can result from genetic mutations, infections, immune system problems, or bone marrow dysfunction. Early diagnosis is essential because children’s bodies are still developing, and untreated blood diseases can affect growth and organ function.
Why Blood Disorders in Children Require Specialised Care
Children are not simply “small adults.” Their blood systems behave differently, and symptoms may appear differently compared to adults.
For example:
- Children with anaemia may show irritability rather than fatigue.
- Bone pain may indicate leukaemia rather than growth pain.
- Frequent infections may signal immune-related blood conditions.
This is why paediatric haematologists receive specialised training to diagnose blood diseases in children and provide treatments tailored to their age and development.
Specialised care ensures that children receive accurate diagnoses, appropriate medications, and long-term monitoring.
Common Childhood Blood Disorders
Several blood disorders occur more frequently during childhood. Understanding these conditions helps parents recognize early symptoms and seek medical care quickly.
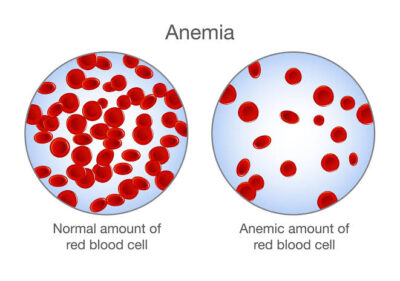
1. Iron Deficiency Anaemia
Iron deficiency anaemia is one of the most common blood diseases in children worldwide. It occurs when the body does not have enough iron to produce healthy red blood cells.
Causes
- Poor dietary intake of iron
- Rapid growth during infancy or adolescence
- Blood loss or chronic illness
Symptoms
- Fatigue
- Pale skin
- Irritability
- Poor concentration
If untreated, iron deficiency anaemia can affect cognitive development and learning ability.
2. Thalassaemia
Thalassaemia is a genetic blood disorder that affects haemoglobin production.
Children with severe thalassaemia may require lifelong blood transfusions and medical monitoring.
Symptoms may include
- Severe anaemia
- Delayed growth
- Bone deformities
- Enlarged spleen
Thalassaemia is particularly common in South Asia, making it a major focus of paediatric haematology Pakistan programs and screening initiatives.
3. Sickle Cell Disease
Sickle cell disease causes red blood cells to become rigid and crescent-shaped. These abnormal cells can block blood vessels and reduce oxygen delivery to tissues.
Symptoms
- Pain episodes
- Fatigue
- Increased infection risk
- Delayed growth
Children with sickle cell disease often require specialized care and preventive treatments to avoid complications.
4. Haemophilia
Haemophilia is a genetic bleeding disorder in which blood lacks certain clotting factors.
Symptoms
- Easy bruising
- Frequent nosebleeds
- Prolonged bleeding after injuries
- Joint swelling
Because bleeding episodes can occur spontaneously, children with haemophilia often require regular clotting factor therapy.
5. Childhood Leukaemia
Leukaemia is the most common type of cancer affecting children. It develops when abnormal white blood cells grow uncontrollably in the bone marrow.
Childhood leukaemia signs include
- Persistent fatigue
- Frequent infections
- Unexplained bruising
- Bone or joint pain
- Swollen lymph nodes
Early detection is critical because prompt treatment significantly improves survival rates.
Age-Specific Symptoms of Blood Disorders in Children
Symptoms of blood disorders can vary depending on a child’s age.
Understanding these differences helps parents recognize warning signs earlier.
Infants (0–12 months)
Blood disorders in infants may present as:
- Poor feeding
- Pale skin
- Slow growth
- Frequent infections
Because infants cannot describe symptoms, subtle changes in behavior or feeding patterns may indicate health problems.
Toddlers and Young Children
Young children may show symptoms such as:
- Irritability
- Low energy
- Bruising or bleeding
- Recurrent infections
Parents should pay attention to unexplained bruises or unusual fatigue.
School-Age Children
In older children, blood disorders may cause:
- Difficulty concentrating in school
- Persistent tiredness
- Bone pain
- Shortness of breath during activity
Recognizing these age-specific symptoms allows earlier diagnosis and treatment.
Childhood Leukaemia Signs Parents Should Watch For
Leukaemia accounts for a large proportion of childhood cancers worldwide. Fortunately, advances in treatment have significantly improved survival rates.
However, early detection remains critical.
Parents should watch for these childhood leukaemia signs:
- Persistent fever
- Fatigue and weakness
- Frequent infections
- Easy bruising or bleeding
- Bone or joint pain
- Swollen lymph nodes
Because these symptoms can resemble common childhood illnesses, medical evaluation is essential if they persist.
How Blood Disorders Are Diagnosed in Children
Doctors use several tests to diagnose blood disorders.
Common diagnostic tests include
Complete Blood Count (CBC)
A CBC measures red blood cells, white blood cells, and platelets to detect abnormalities.
Peripheral Blood Smear
A microscope examination of blood cells helps identify abnormal shapes or structures.
Bone Marrow Examination
Doctors may examine bone marrow to diagnose leukaemia or other bone marrow disorders.
Genetic Testing
Some inherited conditions, such as thalassaemia, require genetic testing for accurate diagnosis.
Early testing allows pediatric haematologist to identify problems before complications occur.
Treatment Options for Childhood Blood Disorders
Treatment depends on the type and severity of the blood disorder.
Common treatment approaches include:
Medications
Certain blood diseases can be managed with medications that stimulate blood cell production or control immune responses.
Blood Transfusions
Children with severe anemia or thalassaemia may require regular transfusions to maintain healthy red blood cell levels.
Clotting Factor Therapy
Children with haemophilia often receive clotting factor infusions to prevent bleeding episodes.
Bone Marrow Transplant
For some conditions, such as leukaemia or severe bone marrow disorders, a bone marrow transplant may offer a potential cure.
Advances in pediatric haematology have dramatically improved treatment outcomes for many children.
The Role of Early Screening in Paediatric Haematology
Screening programs help identify blood disorders before symptoms appear.
Early screening is especially important for genetic diseases such as thalassaemia.
Many countries have implemented newborn screening programs to detect inherited blood disorders early. Early diagnosis allows doctors to begin treatment quickly and reduce complications.
In paediatric haematology Pakistan, improving screening programs and awareness is a major priority.
Supporting Children Living with Blood Disorders
Living with a chronic blood disorder can be challenging for children and their families.
However, proper support can help children lead active and fulfilling lives.
Key support strategies include
- Regular medical monitoring
- Balanced nutrition
- Infection prevention
- Emotional support and counseling
- School support for learning challenges
Parents, doctors, and educators play an important role in helping children manage their condition and maintain a healthy lifestyle.
When Parents Should Seek Medical Advice
Parents are often the first to notice subtle health changes in their children. While occasional fatigue or bruising may not be serious, persistent symptoms should not be ignored.
Many blood diseases in children develop gradually, and early medical evaluation can prevent complications. Paediatricians often recommend blood tests when symptoms persist without an obvious cause.
Parents should consider seeking medical advice if their child experiences:
- Persistent fatigue or weakness
- Pale or yellowish skin
- Frequent infections
- Unusual bruising or bleeding
- Bone or joint pain
- Swollen lymph nodes
- Slow growth or delayed development
These symptoms do not always mean a serious condition, but they may indicate underlying blood disorders that require evaluation by a specialist.
Warning Signs That Require Immediate Medical Attention
Some symptoms may signal serious blood disorders and require urgent medical care.
Severe or Persistent Bleeding
Bleeding that does not stop easily after minor injuries may indicate clotting disorders such as haemophilia or platelet abnormalities.
Frequent High Fevers
Recurring fevers combined with fatigue or bruising may be associated with infections or blood cancers such as leukaemia.
Sudden Weakness or Extreme Fatigue
Extreme tiredness that interferes with normal play, school activities, or eating could be linked to anaemia or other blood conditions.
If any of these symptoms appear suddenly or worsen quickly, parents should consult a paediatrician or haemotology specialist.
Preventing Complications in Childhood Blood Disorders
While some blood disorders are genetic and cannot be prevented, early detection and proper care can reduce complications.
Children diagnosed with blood conditions often benefit from regular monitoring and lifestyle adjustments that support overall health.
Importance of Regular Medical Checkups
Routine medical visits allow doctors to monitor a child’s blood counts, growth, and response to treatment. Regular testing helps detect changes early and adjust treatments when necessary.
For children living with chronic conditions like thalassaemia or sickle cell disease, long-term monitoring is essential.
Nutrition and Blood Health in Children
Proper nutrition plays a key role in maintaining healthy blood cells.
Parents can support their child’s blood health by ensuring a balanced diet that includes:
- Iron-rich foods such as spinach, beans, and lean meats
- Vitamin B12 sources like dairy products and eggs
- Folate-rich foods including leafy vegetables and legumes
These nutrients help support red blood cell production and overall growth.
For children with diagnosed blood disorders, doctors may recommend dietary supplements or specialised nutritional plans.
Emotional Support for Children with Blood Disorders
Living with a medical condition can be emotionally challenging for children. Frequent doctor visits, treatments, or hospital stays may affect a child’s confidence and social development.
Parents and caregivers can support children by:
- Encouraging open communication about their feelings
- Maintaining normal routines whenever possible
- Working closely with teachers and schools
- Seeking counseling if needed
Strong emotional support helps children adapt to their condition and maintain a positive outlook.
The Growing Role of Paediatric Haematology in Pakistan
Over the past decade, medical awareness and diagnostic capabilities for pediatric hematology in Pakistan have improved significantly.
Specialised haematology centers are expanding access to advanced diagnostic tools such as:
- Genetic testing for inherited blood diseases
- Bone marrow analysis
- Advanced laboratory screening for childhood cancers
These advancements help doctors diagnose blood diseases in children earlier and provide more effective treatments.
Specialised institutions and research initiatives are also improving outcomes for children with conditions like thalassaemia and leukaemia.
As awareness grows, parents are increasingly recognizing the importance of early screening and specialist care for childhood leukaemia signs and other paediatric blood disorders.
NIBD Paediatric Haematology :Specialized Care for Children
Early diagnosis and expert treatment can make a life-changing difference for children with blood disorders.
The kids blood disorder NIBD program provides comprehensive diagnostic and treatment services designed specifically for young patients.
The paediatric haematology specialists at NIBD provide advanced medical care tailored to the needs of infants, children, and adolescents.
Parents concerned about symptoms such as unexplained fatigue, frequent infections, or unusual bruising should consult a paediatric specialist for evaluation and testing.
Early care helps ensure the best possible outcomes for young patients.
Frequently Asked Questions
What are the most common blood diseases in children?
Common childhood blood disorders include iron deficiency anaemia, thalassaemia, sickle cell disease, haemophilia, and leukaemia. These conditions affect red blood cells, clotting ability, or the immune system. Early diagnosis and treatment are important to prevent complications and support healthy growth and development.
What are early childhood leukaemia signs?
Early signs of childhood leukaemia may include fatigue, frequent infections, unexplained bruising, bone pain, swollen lymph nodes, and persistent fever. Because these symptoms can resemble common illnesses, medical evaluation is essential if they persist.
How are blood diseases in children diagnosed?
Doctors diagnose blood diseases using tests such as complete blood count (CBC), blood smear analysis, bone marrow examination, and genetic testing. These tests help identify abnormalities in blood cells and determine the specific type of disorder.
Can children recover from blood disorders?
Some blood disorders can be cured, especially with treatments like bone marrow transplantation. Others require long-term management through medication, transfusions, or monitoring. Early diagnosis significantly improves outcomes.
When should parents see a paediatric haematologist?
Parents should consult a paediatric haematologist if a child experiences persistent fatigue, frequent infections, unusual bruising, prolonged bleeding, or abnormal blood test results. Early evaluation ensures timely diagnosis and proper treatment.
Final Thoughts
Blood disorders in children can affect growth, energy, and immunity, but early diagnosis greatly improves outcomes. Recognising symptoms like fatigue, frequent infections, or unusual bruising helps parents seek timely care.
With advances in paediatric haematology in Pakistan and specialised treatment, many children with blood diseases can receive effective care and live healthy, active lives.